Overcoming Rebound Congestion
Understanding Rebound Congestion
When used as directed, topical decongestant nasal sprays are safe and effective medications for the relief of short term nasal congestion. Due to the fact that upper respiratory infections can often last longer than the 3-4 day “safe period” the prolonged use of the sprays can induce rebound congestion which persists long after patients have recovered from the underlying illness.
Rebound congestion first appeared in medical literature in the 1930’s. Prior to the mid-1960’s, decongestant nasal sprays required a prescription. When these medications became available over the counter, rebound congestion began to proliferate.
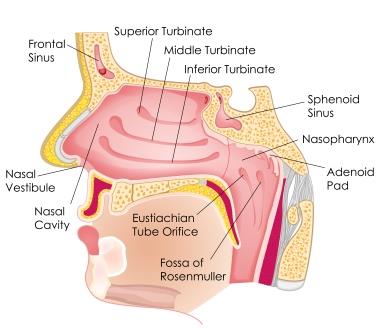
The Challenge of Treatment
The primary treatment for RM is to stop using the decongestant spray altogether. Unfortunately, this can be incredibly difficult. Stopping abruptly leads to a period of intense congestion lasting 4-7 days, deterring many from following through. Traditional medications like steroids, while reducing inflammation, offer no improvement in airflow.
A Comfortable Solution: The Rhinostat System
The Rhinostat System offers a patient-centered approach to overcoming decongestant dependence. It addresses the core challenge of withdrawal discomfort:
Benefits of Gradual Weaning with Rhinostat:
- Gradual Weaning: By precisely tapering medication strength over 2-4 weeks, Rhinostat minimizes congestion during withdrawal, allowing for comfortable breathing.
- Preservative-Free Formulation: Rhinostat kits are free of benzylkonium chloride, a preservative that can worsen RM symptoms.
- Precise Dosage Control: The Rhinostat apparatus allows for gradual reduction in medication, ensuring a smooth transition off decongestant sprays.
Understanding Addiction to Decongestant Sprays
Dependence on decongestant sprays is not a true addiction, as there’s no pleasurable “high” associated with the medication. People become reliant on the sprays because prolonged use causes the nasal passages to swell up, leading to severe congestion when stopped until the nasal passages return to normal size. Contrary to common misconceptions, nasal spray addiction does not involve cravings or a “high” associated with substance abuse. Instead, individuals become dependent on nasal sprays like Afrin to alleviate severe congestion that obstructs airflow. Prolonged use beyond the recommended period can lead to addiction, with withdrawal resulting in complete nasal blockage for 4-7 days. Rhinostat offers a gradual weaning approach to help individuals overcome dependence on decongestant nasal sprays, promoting comfortable airflow during the withdrawal process.
Breaking the Cycle Comfortably
Abruptly stopping decongestant sprays is challenging due to the intense congestion that follows. The Rhinostat System’s gradual weaning approach helps patients overcome dependence comfortably and effectively. Rebound congestion and nasal spray addiction present significant challenges in healthcare, requiring a multifaceted approach to treatment. By understanding the underlying mechanisms and leveraging innovative solutions like the Rhinostat System, patients can overcome dependence on nasal sprays and achieve lasting relief from congestion without compromising airflow.
Important Information:
- How Rhinostat Works
- Learn more about Rhinitis Medicamentosa
- Rhinostat Ordering Information
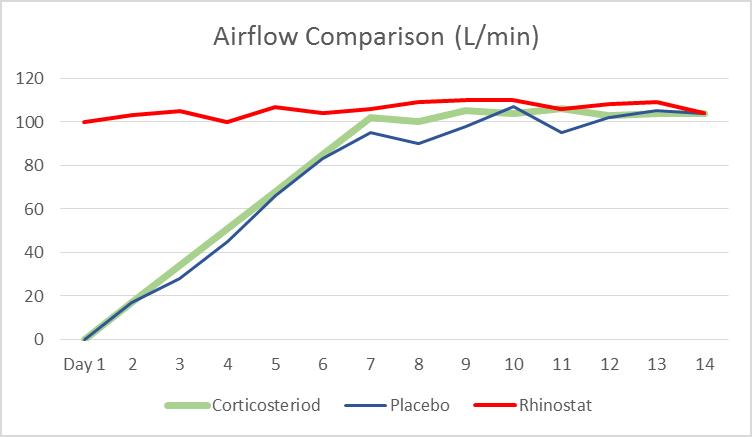
Airflow Comparison Chart: Patients using corticosteroids and placebo experience severely restricted airflow for the first 6-7 days, once the decongestants are withdrawn. Patients who are gradually weaned using Rhinostat maintain comfortable airflow during the entire withdrawal period. All patients have similar airflow after 10-14 days
I just want to thank you from the bottom of my heart for helping me kick the nasal spray habit!!
I have been using nasal spray for about 15 years now. I was using the 12 hour nasal spray about 5 times a day, and then getting up in the middle of the night once to spray again because I couldnt breathe. When I woke up in the morning so stopped up, it would make me cry because it was so frustrating not to be able to breathe through my nose. Everywhere I went, I had to make sure that I had a bottle of spray with me. Even when I had a formal event to go to, I would have my small dress purse with my bottle of nasal spray in it! had a bottle in just about every room in my house including my night stand. I felt like I was trapped for life!
One day, I decided to check the internet for nasal spray addiction. I came across your website and decided to read up on your product. I had no idea that there are that many people in the world that were in the same position as I was. I felt like I was the only one in the world that had this problem. Well, I was determined to make this work for me because I was tired of living that way, being dependent on the spray. At first, I had moments of stuffiness, but within days I had kicked this addiction. I have not had to use a nasal spray in about 2 months. It feels fantastic!! My husband is so proud of me and so am I.
Thanks again, you’ve changed my life.
